Age-related brain disease encompasses a range of conditions that affect cognition and emotional well-being, including stroke, dementia, and late-life depression. Recent research highlights 17 modifiable risk factors that may significantly lower the chances of developing these debilitating disorders. By addressing issues such as high blood pressure, chronic kidney disease, and unhealthy lifestyle choices, individuals can take proactive steps toward improving their brain health. Additionally, understanding the link between these conditions reveals opportunities for preventing stroke and late-life depression. As we navigate the complexities of aging, a targeted brain health assessment can guide us towards effective strategies in preventing these age-related brain diseases.
Age-related cognitive decline, often manifested as dementia or other brain disorders, poses a significant challenge as we grow older. This decline can be influenced by various factors, including lifestyle choices and overall health management. Terminology such as neurodegeneration and age-related cognitive impairment often emerge in discussions regarding the prevention of these conditions. A comprehensive approach that includes addressing modifiable health risks can play a pivotal role in delaying or mitigating the onset of these diseases. By focusing on preventative measures, we can foster not only brain health but enhance overall quality of life in later years.
Understanding Age-Related Brain Disease
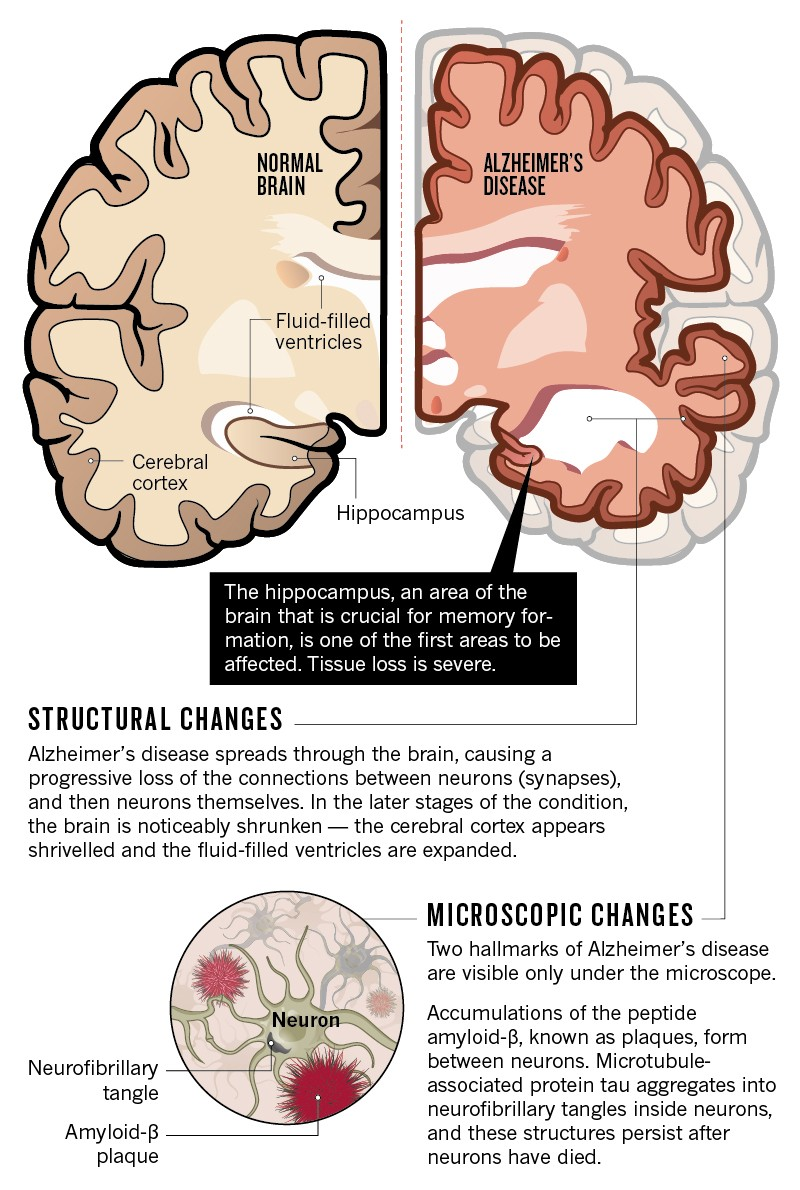
Age-related brain diseases, such as dementia and stroke, have become increasingly prevalent in our aging population. These conditions not only affect cognitive function but also have a profound impact on the overall quality of life for individuals and their families. Researchers have identified a range of modifiable risk factors that may interplay to increase the likelihood of developing age-related brain diseases, offering a pathway for prevention. By implementing lifestyle changes, individuals can significantly reduce their risk and promote better brain health as they age.
The importance of recognizing the interconnectedness of these diseases cannot be overstated. High blood pressure, obesity, and diabetes are just a few of the risk factors highlighted in recent studies as contributors to age-related cognitive decline. When we discuss age-related brain disease, understanding the cumulative risk posed by these factors helps us appreciate the holistic approach needed for prevention. Early interventions and regular health assessments are crucial steps in managing these risks effectively.
Identifying Risk Factors for Dementia
Numerous studies have documented the various risk factors associated with dementia, notably those that are modifiable. Blood pressure and kidney disease feature prominently among these, signifying that regular health monitoring is essential. By addressing these risk factors, such as maintaining a healthy diet and engaging in regular physical activity, individuals can potentially stave off cognitive decline. Awareness around the impact of lifestyle choices has opened new avenues for dementia prevention strategies that could alter disease trajectories significantly.
Moreover, understanding the role of psychological factors, such as stress and late-life depression, is vital in the context of dementia prevention. Late-life depression, for instance, not only exacerbates cognitive decline but also contributes to a vicious cycle of disengagement and further decline. Preventive measures focused on mental health, including fostering social connections and pursuing fulfilling activities, are crucial in addressing these interconnected aspects. Identifying and managing these risk factors can lead to improved brain health assessments and outcomes.
The Role of Modifiable Health Risks
Modifiable health risks play a pivotal role in decreasing the likelihood of developing age-related brain diseases. Conditions such as high blood pressure, obesity, and poor diet can be addressed through lifestyle changes. Incorporating nutrient-rich foods, engaging in consistent physical activity, and adopting stress-reducing practices can significantly mitigate these risks. Current research underscores the findings that even small adjustments in daily habits can yield substantial benefits in overall brain health and reduce the risk of associated diseases.
Additionally, the concept of modifiable health risks serves as a motivational tool for individuals to take charge of their health. With actionable steps outlined by health professionals, people can integrate sustainable changes into their routines. Preventive measures such as regular health screenings and lifestyle interventions not only improve individual health outcomes but also foster a broader understanding of how collective efforts can alleviate the burden of age-related brain disorders.
Preventing Stroke with Lifestyle Changes
Preventing stroke hinges significantly on understanding and addressing modifiable lifestyle factors. Current research suggests that maintaining a balanced diet, engaging in physical activity, and controlling blood pressure can drastically lower stroke risk. The emphasis on modifying behaviors, such as reducing alcohol intake and quitting smoking, is crucial to combat the rising rates of stroke among older adults. These simple yet impactful changes can dramatically enhance long-term brain health outcomes.
Moreover, individuals should prioritize regular health assessments to monitor potential risk factors for stroke effectively. The ongoing dialogue about stroke prevention highlights the importance of community support and resources that promote healthy living. Education plays a critical role, empowering individuals with the knowledge and tools necessary to make informed decisions about their health, therefore preventing potential stroke incidents.
Late-Life Depression Prevention Strategies
Late-life depression remains a critical focus for both mental and physical health due to its strong association with other age-related brain diseases. Prevention strategies target various aspects impacting well-being, such as social engagement and sense of purpose in life. Engaging with community resources and participating in meaningful activities can drastically improve mental health outcomes for older adults. Regular social interactions can provide emotional support and reduce feelings of isolation, which are often prevalent in this demographic.
Additionally, healthcare providers should emphasize the importance of mental health evaluations as part of regular health assessments. By identifying and addressing mental health issues early, healthcare professionals can implement effective interventions that may prevent the onset of late-life depression. The interplay of mental and physical health is crucial, and comprehensive strategies that encompass both aspects will be vital for successful prevention and intervention.
The Importance of Brain Health Assessment
Conducting regular brain health assessments is essential for identifying risks associated with age-related brain diseases. These assessments encompass evaluations of cognitive function, lifestyle habits, and medical history, helping healthcare providers determine individual risk profiles. The recent introduction of tools like the Brain Care Score has streamlined this process, offering a systematic approach to monitoring brain health and determining areas for improvement.
Moreover, the role of technology in facilitating brain health assessments cannot be ignored. Advances in medical technology are allowing for more precise tracking of biomarkers and cognitive functioning. As researchers continue to explore the relationship between various risk factors and cognitive decline, the relevance of routine assessments will only become more pronounced, making early detection and intervention significantly more achievable.
Strategies for Healthy Aging
Adopting strategies for healthy aging is crucial in mitigating the risks associated with age-related brain diseases. Individuals are encouraged to focus on a holistic approach that includes physical, mental, and social wellness. Regular exercise, a balanced diet, and mental exercises are not only beneficial but necessary for maintaining cognitive health. Engaging in activities that challenge the brain, such as learning new skills or solving puzzles, can foster cognitive resilience.
Moreover, social engagement is equally important for healthy aging. Building and maintaining robust social networks can provide the necessary emotional and psychological support that contributes to overall health. Encouraging older adults to participate in community activities or volunteer work can significantly enhance their wellness and sense of belonging, which is also a protective factor against various age-related cognitive impairments.
Impacts of Chronic Pain on Brain Health
Chronic pain presents a dual challenge for brain health, significantly impacting both physical and mental well-being. It’s linked to elevated risks of depression, which can exacerbate cognitive decline and increase the incidence of age-related brain diseases. Understanding how chronic pain affects quality of life is paramount; as individuals experience persistent discomfort, their ability to engage with activities that promote brain health diminishes.
Addressing chronic pain requires a comprehensive approach involving medical interventions, lifestyle adjustments, and psychological support. Management strategies that incorporate pain relief while encouraging physical activity can improve overall health outcomes. Such initiatives not only aim to reduce pain but also enhance engagement with cognitive activities, fostering a more proactive approach to brain health.
The Interconnection Between Brain Disorders
The interconnection between cognitive disorders such as stroke, dementia, and late-life depression is an emerging area of research importance. Understanding how these conditions overlap allows for the development of cohesive prevention strategies that target multiple risks simultaneously. For instance, addressing high blood pressure not only helps in stroke prevention but also contributes to lowering dementia risk. This systematic approach underscores the value of treating the individual holistically rather than in isolation.
Furthermore, the recognition of shared risk factors among these disorders highlights the need for multidisciplinary teams in healthcare. By bringing together expertise across various fields, there’s an opportunity to create comprehensive care plans tailored to individual needs. Such collaborative efforts are crucial for developing targeted interventions that address the root causes of age-related brain diseases, ultimately leading to better health outcomes.
Frequently Asked Questions
What are the main risk factors for age-related brain disease such as dementia and stroke?
The main risk factors for age-related brain disease, including dementia and stroke, include high blood pressure, diabetes, kidney disease, and lifestyle choices such as poor diet, lack of physical activity, smoking, and excessive alcohol use. Additionally, modifiable factors like social engagement, sleep quality, and the presence of chronic pain also play significant roles.
How can modifying health risks lower the chances of age-related brain diseases?
Modifying health risks such as hypertension, diabetes, and lifestyle factors can significantly reduce the likelihood of developing age-related brain diseases like dementia and stroke. The study from Mass General Brigham shows that even changes in one modifiable risk factor can lead to improved outcomes for brain health.
What role does diet play in preventing stroke and dementia?
Diet is a crucial modifiable health risk for preventing stroke and dementia. An unhealthy diet can increase the risks of both conditions, while a nutritious, balanced diet helps support overall brain health and lower the risk of cognitive decline and vascular issues.
What is the significance of ‘purpose in life’ in preventing late-life depression related to age-related brain disease?
Having a sense of purpose in life is linked to lower rates of late-life depression, which in turn can lessen the risk of developing age-related brain diseases. Engaging in meaningful activities can enhance mental well-being and serve as a protective factor against cognitive decline.
How does chronic stress influence the risk of age-related brain disease?
Chronic stress is a significant modifiable risk factor that can elevate the risk of age-related brain diseases such as dementia and depression. It negatively impacts mental health and can exacerbate underlying health issues, making stress management essential for maintaining brain health.
Why are lifestyle changes important in preventing age-related brain diseases?
Lifestyle changes are critical in preventing age-related brain diseases because many risk factors, such as physical inactivity, smoking, and unhealthy eating, can be modified. The Mass General Brigham research emphasizes that addressing these risk factors can significantly improve brain health and lower the incidence of diseases like stroke and dementia.
What is the Brain Care Score and how does it relate to preventing age-related brain disease?
The Brain Care Score is a tool developed by researchers at Mass General Brigham to assess brain health and guide individuals in making lifestyle changes. It incorporates findings regarding modifiable health risks for age-related brain diseases, aiming to provide a framework for improving overall brain function and reducing disease risk.
How does social engagement affect the risk of age-related brain diseases?
Social engagement is a critical factor in reducing the risk of age-related brain diseases. Isolation can lead to increased rates of late-life depression and cognitive decline, while active social participation promotes mental stimulation and emotional well-being, thus supporting brain health.
Can improving physical activity levels reduce the risk of dementia and stroke?
Yes, enhancing physical activity levels is linked to a reduced risk of dementia and stroke. Regular exercise not only supports cardiovascular health but also contributes to better cognitive function, making it an essential factor in maintaining brain health during aging.
What are some effective strategies for preventing late-life depression in older adults?
Effective strategies for preventing late-life depression include maintaining social connections, staying physically active, ensuring a balanced diet, managing stress, and finding purpose through engaging in hobbies or volunteering. Addressing these areas can significantly enhance mental health and mitigate the risk of age-related brain diseases.
| Risk Factor | Associated Conditions | Impact on Health |
|---|---|---|
| Diabetes | Stroke, Dementia, Depression | Increases overall risk for all three conditions |
| High Blood Pressure | Stroke, Dementia, Depression | Significantly heightens risk and incidence |
| Kidney Disease | Stroke, Dementia, Depression | Elevates risk levels across multiple conditions |
| Fasting Plasma Glucose | Stroke, Dementia, Depression | Increases risk associated with blood sugar levels |
| Total Cholesterol | Stroke, Dementia | Raised cholesterol can lead to higher stroke risk |
| Alcohol Use | Stroke, Dementia, Depression | Excessive intake correlates with increased risks |
| Diet | Stroke, Dementia, Depression | Poor dietary habits can trigger health issues |
| Hearing Loss | Dementia | Modifiable factor that can influence risk |
| Chronic Pain | Depression | May exacerbate depressive symptoms and risks |
| Physical Activity | Stroke, Dementia, Depression | Lack of activity significantly increases risks |
| Sense of Purpose | Depression | A sense of purpose helps mitigate risks |
| Sleep Quality | Depression | Poor sleep can worsen depressive symptoms |
| Smoking | Stroke, Dementia, Depression | Major contributing factor across conditions |
| Social Engagement | Depression | Isolation can lead to worsened conditions |
| Chronic Stress | Depression | Leads to higher risks for multiple disorders |
| Obesity | Stroke, Dementia, Depression | Recognized risk factor influencing overall health |
Summary
Age-related brain disease encompasses a spectrum of conditions that can significantly impact quality of life in older adults. Research identifies a wide array of modifiable risk factors that can be targeted to mitigate the decline associated with such diseases. By addressing these factors—ranging from blood pressure and physical activity to social engagement and diet—individuals may reduce their chances of developing debilitating conditions like stroke, dementia, and late-life depression. Preventive measures are crucial, as the overlap in risk factors presents unique opportunities for comprehensive health strategies aimed at maintaining cognitive and emotional well-being as people age.